May 2022
Am J Respir Crit Care Med
Inhaled iloprost improves right ventricular load-independent contractility in pulmonary hypertension
Abstract
The efficacy of prostacyclin therapy in pulmonary arterial hypertension (PAH) may be partly related to positive inotropic effects on the right ventricle (RV), but this has been difficult to demonstrate in vivo. We compared the acute effects of inhaled iloprost (2.5 μg) and inhaled nitric oxide (NO; 10 ppm) or orally administered riociguat (1 mg) on RV contractility defined by load-independent pressure-volume relationships in patients with PAH (n = 19, 8, and 5, respectively). RV pressures and volumes were measured using gold-standard high-fidelity conductance catheters. Contractility (end-systolic elastance [Ees]) and afterload (arterial elastance [Ea]) were determined using multiple-beat methods. Ea decreased from baseline with both iloprost and NO/riociguat, but iloprost increased median Ees (from 0.56 [interquartile range: 0.40–0.79] mm Hg/ml to 0.63 [0.53–0.90] mm Hg/ml; P < 0.001) whereas NO/riociguat decreased Ees (from 0.70 [0.51–1.04] mm Hg/ml to 0.59 [0.45–0.74] mm Hg/ml; P < 0.001). Both iloprost and NO/riociguat increased RV ejection fraction (EF), but only iloprost increased cardiac output. We were also able to confirm the inotropic effect of iloprost in 12 rats with pulmonary arterial banding (PAB). In conclusion, our results strongly suggest that inhaled iloprost acutely increases RVEF and cardiac output in patients with PAH by a combination of decreased afterload and increased RV contractility.
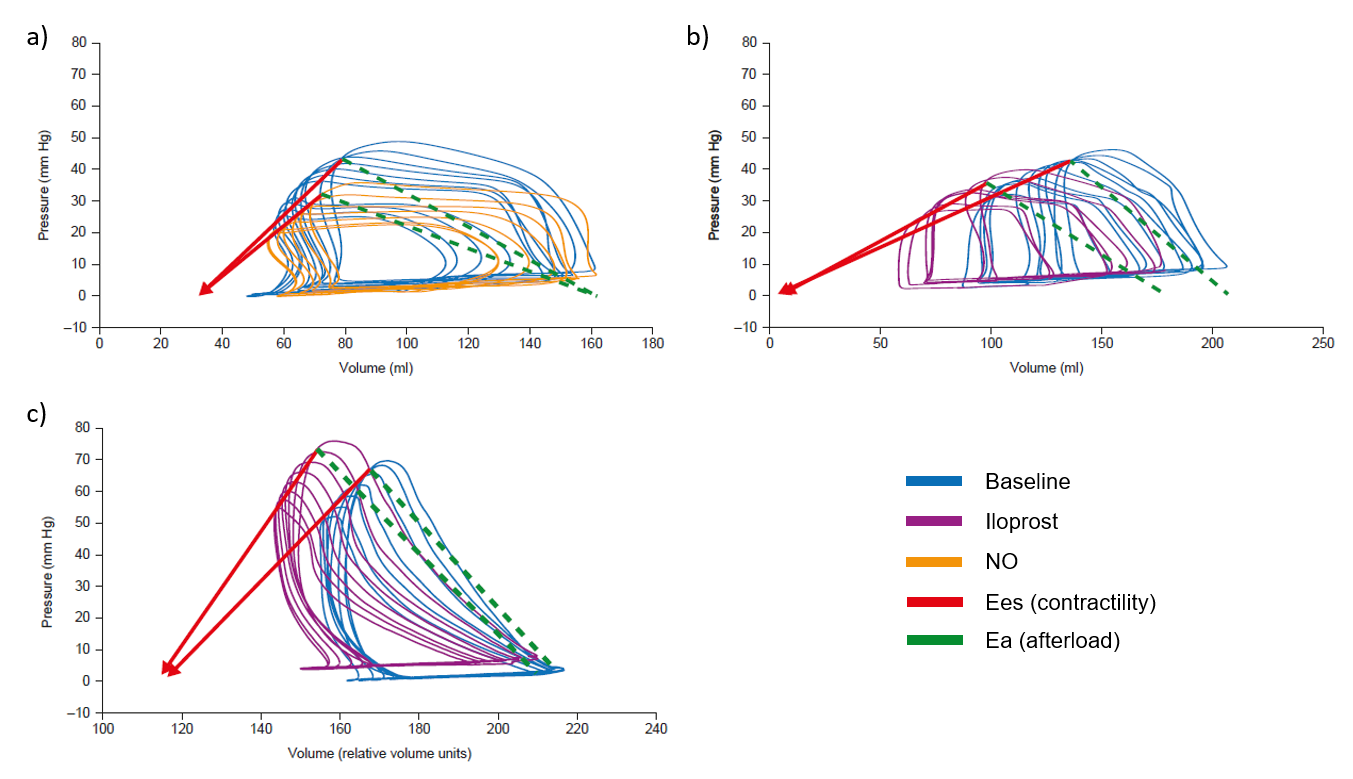
Legend to graphical abstract:
Effect of iloprost and nitric oxide on right ventricular function. Example pressure-volume loops are shown for (A) a patient with PAH before and during nitric oxide inhalation, (B) a patient with PAH before and after iloprost inhalation, and (C) a rat with pulmonary arterial banding before and after iloprost infusion. Right ventricular contractility (Ees) was increased after iloprost inhalation or infusion but decreased during nitric oxide inhalation. The slope of the solid red straight lines indicates Ees; the slope of the dashed green straight lines indicates Ea. Ea = arterial elastance; Ees = end-systolic elastance.